If you’re wondering how long you can stay on Ozempic or Mounjaro, the answer depends on your goals, health, and how your body responds. Some people use these medications for a few months, while others stay on them for years—especially for long-term weight management or diabetes care. Knowing when to continue, adjust, or stop treatment is key to maintaining results safely.
At BODYWELLE in Miami Beach, Dr. Alonso Martin provides weight management services through his customized approach based on patients’ health progress and needs. The increasing use of GLP-1 medications by people requires healthcare professionals to address three main concerns, which include long-term medication usage, potential side effects and treatment effectiveness after patients begin Ozempic.
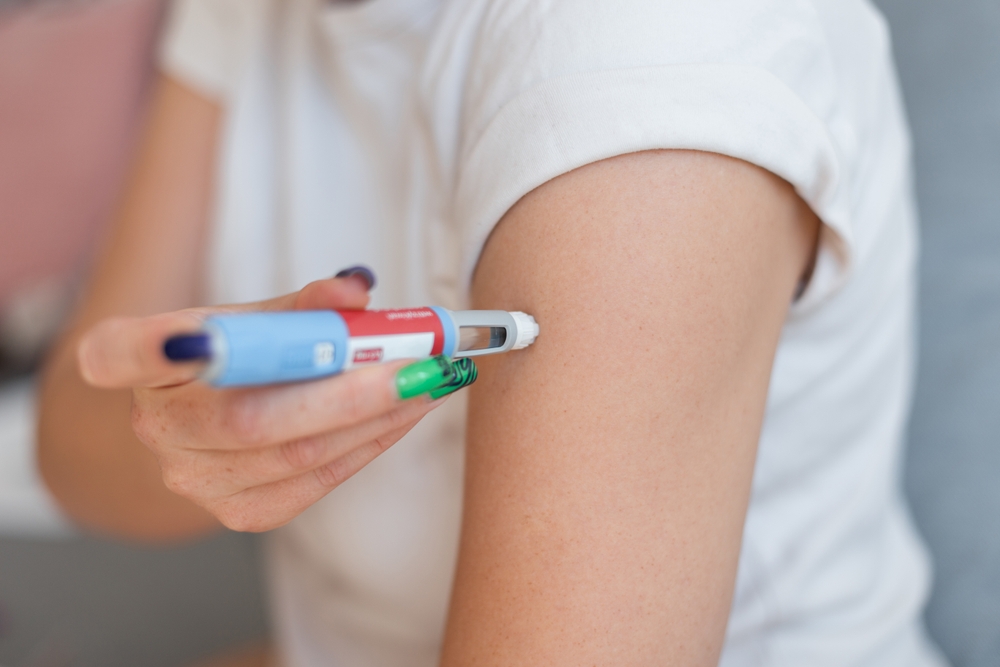
Key Takeaways
- Most people stay on Ozempic or Mounjaro for 6 to 24 months, but some use them longer
- These medications can be used long-term if they remain safe and effective
- Weight loss is typically fastest in the first 3–6 months, then slows over time
- Stopping treatment may lead to increased appetite and possible weight regain
- The ideal duration depends on your goals, health, and medical guidance
How Long Can You Stay on Ozempic for Weight Loss?
Most people use Ozempic for weight loss for 6 to 24 months, though some may stay on it longer if needed. When used for diabetes, it’s often taken long-term. There is no strict time limit as long as the medication remains safe and effective.
- Listen to your body: Mild side effects like nausea or stomach aches usually get better with time. If they’re too strong, your doctor might lower your dose or stop the medication.
- Think about your goals: If you’re using it for weight loss, you might stay on it until you hit your goal — and maybe a bit longer to help keep the weight off. For diabetes, many people stay on it long-term to keep blood sugar steady.
- Talk to your doctor: They’ll check in on you, look at your labs, and make sure the medication is still right for you.
- Everyone’s different: Some people need it for a few months, others for years. Your health, progress, and how you feel will help guide the decision.
How Long Can You Stay on Mounjaro?
Mounjaro can be used long-term as long as it remains safe and effective under medical supervision. Many people stay on it for several months to years, depending on their response to treatment and overall health. There is no fixed time limit for how long you can take it.
- No official time limit: You can stay on Mounjaro as long as it’s working for you and your doctor thinks it’s safe.
- Regular check-ins: Your doctor will want to see how you’re doing and adjust things if needed.
- Maintenance mode: After you hit your goal weight, you might stay on a smaller dose to help keep the weight off.
- Research shows it works long-term: Studies show people can keep losing weight for up to 88 weeks (almost two years!).
- It’s personal: Your plan depends on your starting weight, health, and how well you’re keeping up with diet and exercise.
What to Expect Over Time on Ozempic or Mounjaro
Over time, Ozempic and Mounjaro lead to changes in appetite, weight, and metabolism that happen in phases. Most people see the fastest results early on, followed by steady progress and eventually a plateau as the body adapts to the medication. Looking at an Ozempic results timeline week by week can help patients understand how these phases usually unfold.
- In the first few months:
- By 3-6 months:
- By the 6-12 month mark:
- In long-term users (18 months or longer):
- Appetite and cravings drop noticeably
- You may lose 5-10% of your starting weight
- Blood sugar levels stabilize
- Weight loss continues at a steady pace
- Eating habits and portion control improve
- Weight loss often reaches 15% or more in some patients
- Digestion may slow, and some people experience constipation or mild gastrointestinal effects
- You may need to adjust your dose as your body acclimates
- Weight loss may plateau
- Appetite may slowly return if habits haven’t changed
- Some people experience diminishing returns or side effects like fatigue or nausea
Dr. Martin monitors every stage closely to ensure patients stay on the right dose, receive lab testing as needed, and avoid significant side effects or nutritional deficiencies.
Start Your Journey to Success, Don’t Wait Any Longer!
Join our satisfied clients who’ve experienced safe, effective treatments.
What Are the Long-Term Effects of Ozempic or Mounjaro?
Long-term use of Ozempic or Mounjaro can support ongoing weight management, improved blood sugar control, and overall metabolic health. Some people may also notice changes in how their body responds over time, including slower progress or mild side effects.
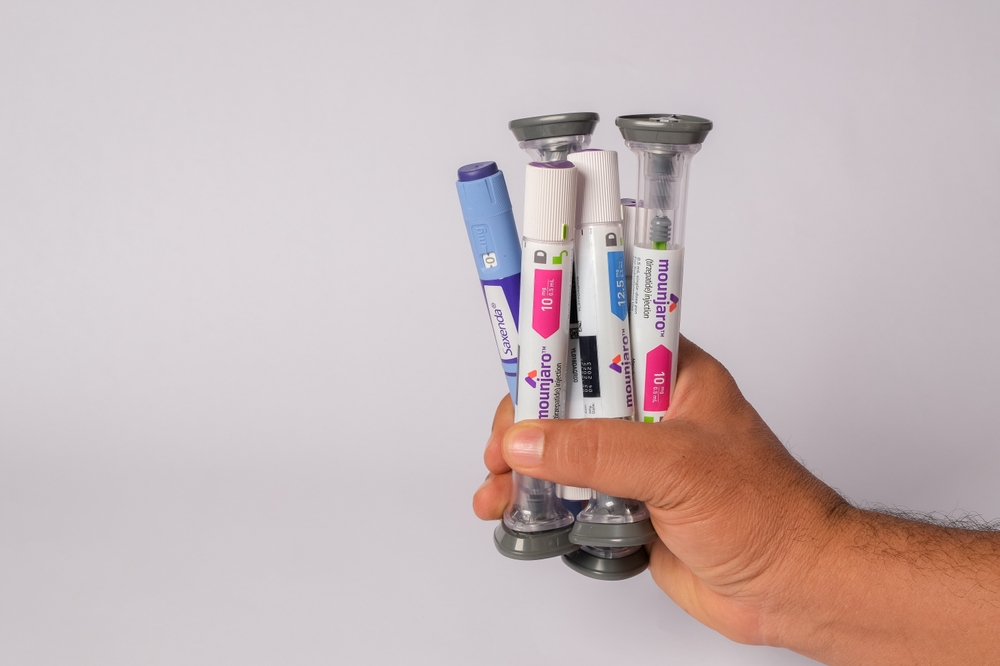
- Continued appetite suppression and weight loss: Many patients experience reduced hunger and steady weight management while staying on the medication.
- Weight loss plateau over time: It’s common for progress to slow or stabilize as your body adapts, even if you continue treatment.
- Improved metabolic markers: Patients often see reductions in A1C, cholesterol, and blood pressure.
- Increased satiety after meals: Because these drugs delay gastric emptying, you may feel fuller for longer.
Dr. Martin helps patients monitor these effects and adjust as needed, ensuring medications are paired with nutrition counseling, exercise, and appropriate lab monitoring. Long-term use may be suitable for some individuals, while others may transition off or switch drugs depending on goals and response.
In some cases, patients may also experience changes in their energy levels, digestion, or mental clarity over time. GLP-1 medications can influence hormone signaling in ways that affect sleep, inflammation, and even mood. This is why a monitored, medical approach is essential—tracking your symptoms and lab values ensures any subtle shifts are addressed early.

Why It Matters How Long You Stay on Weight Loss Injections
Medications like Ozempic (semaglutide) and Mounjaro (tirzepatide) are designed to support significant weight loss over time by reducing appetite, slowing gastric emptying, and helping regulate blood sugar levels. They work by mimicking naturally occurring hormones (GLP-1 or GLP-1/GIP) that act on the brain and gut, helping control hunger, improve insulin sensitivity, and influence how your body uses energy. But these results don’t happen overnight, and staying on the medication for the right length of time plays a critical role in long-term success.

Weight loss is rarely just about the number on the scale. For many patients, it’s about reducing the health risks of obesity—such as high blood pressure, insulin resistance, sleep apnea, and chronic inflammation. Long-term weight management may involve using GLP-1 drugs as a bridge toward better habits and more sustainable health outcomes.
When patients stop taking their medication too soon, weight regain after stopping Ozempic can be common. The body may revert to its previous appetite patterns, and without continued support through medication, diet, and exercise, it becomes much harder to maintain progress. Understanding how long you can stay on Ozempic or Mounjaro—and how long you should—is essential to achieving meaningful, lasting change.
What Happens When You Stop Ozempic or Mounjaro
When you stop Ozempic or Mounjaro, appetite often returns and weight regain is common without lifestyle support. Blood sugar levels may also rise in some individuals, though most side effects improve after stopping.
Discontinuing weight loss medication is a personal decision that should be made with your physician’s guidance. It’s important to know what to expect:
- Appetite may increase: Without the drug suppressing hunger, cravings can return.
- Weight regain is common: Clinical trials show that most people regain some or all of the lost weight within a year of stopping.
- Blood sugar levels may shift: If you have prediabetes or type 2 diabetes, stopping the medication may affect your glucose control.
- Energy levels may change: Some patients feel more tired or experience mood fluctuations post-discontinuation.
However, this doesn’t mean you’re destined to regain the weight. At BODYWELLE, we help patients taper off gradually and replace medication with evidence-based strategies like structured lifestyle planning, medical-grade supplementation, and regenerative treatments that support metabolism.
Some patients may benefit from switching to an alternative GLP-1 medication or considering peptide therapies or nutritional supplements to help bridge the gap. The key is to plan a structured transition, not stop abruptly. In addition, resistance training, protein-focused diets, and stress management can play a large role in preventing rebound weight gain.
When Should You Stop or Switch Ozempic or Mounjaro?
There’s no one-size-fits-all answer for how long can I be on Ozempic for weight loss. Some patients remain on it (or Mounjaro) for years. Others may reach their goal weight and want to transition off. A personalized approach is key.
You may want to consider stopping or switching medications if:
- You’ve reached your weight loss goals and can maintain them with healthy lifestyle changes
- You’re experiencing persistent side effects (like nausea, bloating, or fatigue)
- Your results have plateaued for 6+ months despite consistent dosing
- Bloodwork suggests inflammation, liver changes, or other risks
- You’re preparing for pregnancy (these medications are not safe during pregnancy)
At BODYWELLE, medication is always part of a larger strategy—not a long-term crutch. Dr. Martin uses advanced biomarker testing and body composition analysis to determine when it’s time to reduce or stop injectable medications, and what alternatives may help you stay on track.
Signs Your Treatment Plan May Need Adjustment
Every body responds differently to weight loss medication. That’s why Dr. Martin takes a personalized approach, adjusting dosage, combining therapies, or suggesting new treatments like Emsculpt NEO or metabolic health panels when needed.
Your plan may need adjustment if you notice any of the following:
- Weight loss has completely stalled for 3-6 months
- You’re experiencing new or worsening gastrointestinal symptoms
- You’re having difficulty staying consistent with dosing or injections
- You feel fatigued or emotionally drained
- You’re approaching a goal weight but unsure how to maintain it
You may also want to reassess your goals. For some patients, weight loss is just one part of a broader effort to optimize energy, reduce inflammation, or prevent chronic disease. In those cases, shifting to a long-term wellness plan that includes hormonal health optimization, nutrition support, or mitochondrial function testing may offer even better outcomes.
Hear From Others Using Weight Loss Injections Long-Term
Many patients at BODYWELLE have found success using Ozempic, Mounjaro, Wegovy, or Zepbound as part of their weight loss journey. Some highlights from real-life cases include:
- Patients who lost over 20% of their body weight in a year and kept it off through a combination of medication, strength training, and peptide therapy
- Clients who transitioned from Ozempic to another GLP-1 drug after a plateau and resumed progress
- Individuals with prediabetes who normalized blood sugar levels and avoided progression to diabetes through medication and lifestyle changes
These success stories show what’s possible when medication is

Medical Weight Loss Support at BODYWELLE
GLP-1 medications like Ozempic and Mounjaro have changed the way we approach obesity and chronic weight management. The treatments show strong effectiveness but require implementation through a comprehensive medical program for their results to endure.
At BODYWELLE in Miami Beach, Dr. Alonso Martin specializes in metabolic and hormonal health, using advanced testing and personalized strategies to guide treatment decisions over time. This includes adjusting medication, monitoring lab work, and integrating nutrition, exercise, and other therapies to support sustainable results.
If you’re wondering how long you should stay on Ozempic or Mounjaro, getting individualized guidance is key.
To learn more about our weight loss program or schedule a consultation, visit BODYWELLE or speak with a member of the care team.
Frequently Asked Questions About Ozempic and Mounjaro
How long can you take Ozempic or Mounjaro for weight loss?
Most patients take these medications for 6 to 24 months, though some continue longer depending on their progress and ability to maintain results.
Do you have to take Ozempic forever?
Not necessarily. Some people stop after reaching their goals, while others continue long-term to maintain weight loss or manage blood sugar.
How do drugs like Ozempic compare to other weight loss medications?
GLP-1 receptor agonists such as Ozempic and Mounjaro are among the most effective options currently available for weight loss. Compared to older appetite suppressants or pill-based treatments, these injectable medications tend to produce greater average weight loss and more favorable metabolic outcomes. They work by mimicking gut hormones that regulate hunger, fullness, and blood sugar, and are often better tolerated than many drugs used in the past. However, they must be prescribed and monitored carefully due to potential side effects such as low blood sugar, nausea, or fatigue.
What are the common side effects and potential risks?
Most patients experience mild and manageable side effects, especially early in treatment. Common effects include nausea, constipation, bloating, and fatigue. More serious risks are rare but may include pancreatitis or gallbladder issues, so medical monitoring is important.
Is Ozempic or Wegovy better for weight loss?
Ozempic and Wegovy contain the same active ingredient (semaglutide), but Wegovy is FDA-approved specifically for obesity, while Ozempic is approved for type 2 diabetes. Many patients use Ozempic off-label for weight loss under medical supervision. In clinical trials, Wegovy has shown significant weight loss benefits in people without diabetes. Your doctor will help determine whether Ozempic or Wegovy—or another similar drug—is the right fit for your body mass index, health history, and goals.
How long can you be on Ozempic or Mounjaro?
The duration of treatment varies depending on each patient’s response, goal weight, and medical conditions. Many people take these medications for 12 to 24 months, while others may remain on them longer, especially if they have severe obesity or diabetes. A gradual taper may be advised if you reach your goal weight and can maintain it with healthy lifestyle changes. Regular check-ins with your doctor are essential to evaluate progress and avoid unnecessary adverse effects.
Should I consider bariatric surgery instead of weight loss medication?
Bariatric surgery is typically reserved for individuals with a higher body mass index (usually 40+, or 35+ with serious health issues). If you’ve tried many drugs, diet changes, and lifestyle interventions without long-term success, surgery may be an option. However, medications like Ozempic can offer significant weight loss without the surgical risks or recovery time. Consulting both a bariatric surgeon and a physician experienced in non-surgical options can help you decide the safest and most effective path forward.
Can Ozempic be combined with other medications or supplements?
In some cases, yes—but combinations must be medically supervised. Some patients may benefit from using similar drugs in rotation, or combining GLP-1 medications with peptide therapies or metabolic supplements. However, taking multiple medications increases the chance of interactions or hypoglycemia (low blood sugar). Dr. Martin tailors each treatment plan based on clinical data, your current prescriptions, and your specific metabolic profile.
Are there pill versions of these weight loss drugs?
Currently, most GLP-1 medications for weight loss, including Ozempic and Mounjaro, are available only as injectable treatments. Novo Nordisk has developed an oral form of semaglutide, primarily marketed for diabetes under the brand name Rybelsus. While convenient, the pill form may not be as potent for weight loss as the injectable version. Your doctor can offer advice on whether an oral GLP-1 is appropriate based on your needs.
What should I do if I miss a dose?
Take it as soon as possible within 5 days, then continue your regular schedule. If more time has passed, skip the dose and do not double up. Never double-dose. Talk to your physician for guidance on missed doses and proper drug administration to reduce the risk of adverse effects.
What happens if my body stops responding?
It’s possible to develop a tolerance or reach a weight loss plateau. If your progress slows for more than 3-6 months despite consistent drug use, your doctor may recommend adjusting the dosage, switching to a similar drug, or incorporating other therapies. It’s also a good time to reassess your lifestyle habits, nutrition, and physical activity. Long-term success comes from using these tools in combination—not relying on one medication alone.
Is this treatment safe for everyone with excess weight?
While drugs like Ozempic are effective for weight loss, they’re not appropriate for every person with excess weight. People with certain medical conditions—including a history of pancreatitis, thyroid cancer, or severe gastrointestinal disease—may not be good candidates. That’s why BODYWELLE takes a medical, individualized approach. Through lab testing, health screenings, and personalized advice, we help determine whether GLP-1 therapy or other options are safest for your long-term success.